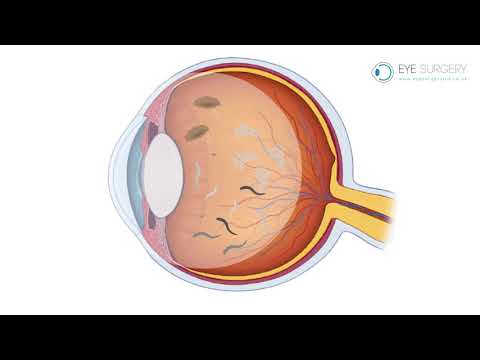
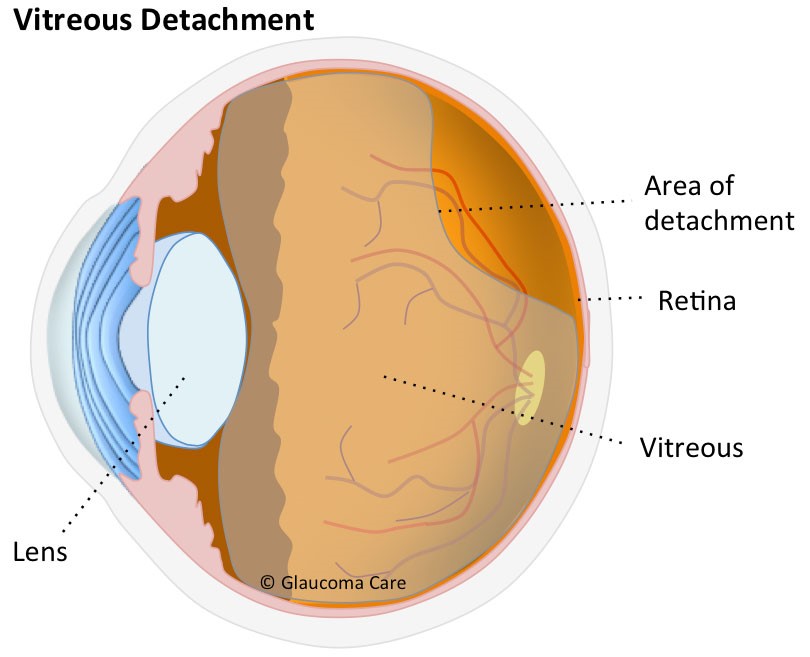
The eye is principally divided into two separate compartments, the front or ‘anterior chamber’ which is filled with aqueous fluid, and the back or ‘posterior chamber’ which is filled with vitreous gel. When you are born this vitreous gel fills the whole posterior chamber of the eye and is glued to the lining of the eye, including the retina and optic nerve. As we all age this vitreous gel slowly dissolves and shrinks. This dissolving gives rise to debris or ‘floaters’ within the gel. These floaters are noticeable when looking at bright lights or even coloured backgrounds as blobs or ‘amoeba’ that move across our vision. As the gel continues to shrink over time it can no longer fill the whole posterior chamber, and at some stage in mid-life it naturally separates from the lining of the eye, and collapses into a small ball of gel. During this process, as the gel pulls free from the retina, it activates the retina and, causes characteristic bright momentary flashes of light. These flashes of light are part of the normal vitreous separation and are nothing to worry about. Eventually, when the gel has completely separated from the back of the eye, you are said to have had a posterior vitreous detachment (PVD). The development of a PVD is a normal process and occurs in everyone! When this occurs more floaters may suddenly appear. These floaters are not normal floaters within the gel, but are larger and more prominent, and represent the back surface of the gel itself. This was previously attached to the retina and was invisible, but after a PVD it floats in front of the retina with eye movement and can intermittently obscure vision. People describe a PVD as like seeing a ‘cobweb in front of the vision,’ or like a ‘road map’. Over time these floaters settle with gravity. They will never fully disappear, and may always be visible when looked for.
Is it advisable to have flashes and floaters checked?
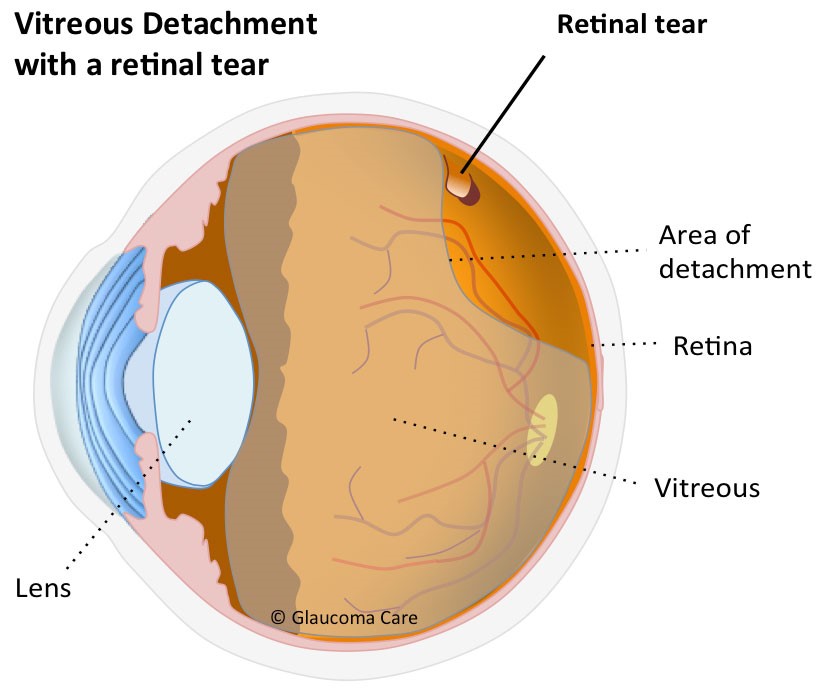
Yes. As with all things in nature, the development of a PVD may not go entirely smoothly. As the vitreous separates from the retina there is a danger that the vitreous is too adherent at one point, causing the blood vessel or retina that the gel is trying to separate from to tear. If a tear is not treated quickly it may develop into a detached retina. This may cause permanent loss of vision. For this reason ophthalmologists advice that if you notice a sudden increase in floaters, known as a ‘shower of floaters’, or a shodow in the vision coming from the edge of the eye, like a curtain coming across the vision, to have your retina checked by an ophthalmologist within 24 hours. A torn retina may turn into a retinal detachment within days if untreated. Simple tears can be lasered in clinic, retinal detachments require an operation to repair. If the central retina has detached, the vision may be become permanently impaired.
Can I have my floaters removed?
Unless floaters represent an underlying problem with the eye, such as a detached retina, they are entirely harmless. If you can learn to ignore them, then it is best option, to leave them alone. If however the floaters are very troublesome and obscure your vision for important tasks such as reading or driving, then they can be removed with a vitrectomy. This is a simple day-case procedure that can be done whilst you are awake. It takes 20 minutes. A pad is worn for 1 night and drops are given for 1 month. However, unlike floaters, operations are not harmless. 1 in 100 people that have a vitrectomy can develop a detached retina or other problem with sight. For this reason we only recommend a vitrectomy if you are significantly troubled by your floaters.